Should the United Nations Office for the Coordination of Humanitarian Affairs estimates prove true, some 274 million people worldwide will need humanitarian aid in 2022 alone.
Some of that needed aid will come from sudden emergencies—the earthquake in Papua New Guinea, flooding in Pakistan, or wildfires in Kazakhstan, for example. Other needed aid will come in direct response to complex humanitarian emergencies, like the hunger crisis in the Horn of Africa and the humanitarian crisis in Ukraine spawned by the Russian invasion.
For more than a decade Team Rubicon has stepped up to help meet the immediate needs of persons across the globe affected by conflict and natural and climate disasters. In doing so, teams on the ground quickly recognized that the best aid given goes beyond the short term: working in tandem with local leaders builds capacity for vulnerable communities and helps make them more resilient in the long term. Providing local individuals and medical care providers with advanced training in lifesaving technologies and techniques, and with access to new technologies, could make a difference for decades.
Such training and advancement in skills is known as capacity building, and in conflict zones and complex disaster situations it can save lives far into the future, long after humanitarian aid from the outside is gone.
What is Capacity Building in Complex Humanitarian Crises?
At Team Rubicon, capacity building is built into our response, recovery, and resilience model. When the organization’s volunteers, known as Greyshirts, arrive in a disaster zone or crisis area, they use their invaluable skills to help people affected in the immediate—they deliver medical aid, provide manpower to clear debris and help return persons to safe living situations, and offer expertise on issues such as logistics.
When it comes to humanitarian aid, capacity building equips communities with the knowledge, technology, and resources to create systems, skills, and mindsets that can sustain continued growth and healing. Using training to equip those who live in the area with advanced skills that can be used into the future builds capacity and resilience in the community.
In Ukraine, a Case Study in Capacity Building
During its initial response to the humanitarian crisis in Ukraine in the spring of 2022, Team Rubicon provided medical support to Internally Displaced Persons (IDPs) at the direction of the World Health Organization and Ukraine Ministry of Health at a hospital in Western Ukraine. EMT Type Mobile 1 teams, in coordination with the Ukraine Ministry of Health, assisted with logistics support and medical care needs.
While there, the organization recognized that capacity building in Ukraine was critical. Given the ongoing nature of the conflict, care for wounded persons and for the everyday medical needs of IDPs was guaranteed to continue, even after humanitarian aid organizations departed.
To ensure that capacity building, Greyshirts returned to Ukraine in August of 2022 with a refined focus of training Ukrainian healthcare professionals and civilians in technology and techniques that could allow them to save lives far into the future. The goal was to expand specialized medical capacity within the Ukrainian healthcare system as it relates to conflict and emergency medicine to help reduce potentially preventable morbidity and mortality, alleviate suffering, and to maintain human dignity during this time of war.
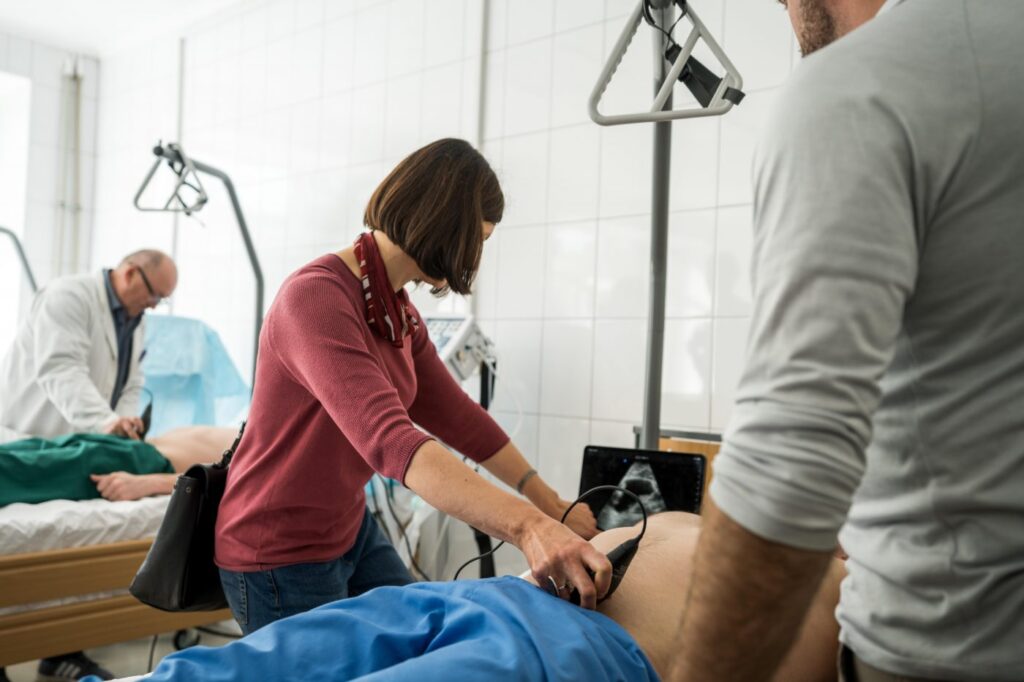
In conflict zones, immediate crisis response needs are regularly ongoing and evolving. Having people at the local level capable of meeting those needs can mean the difference between an injured person receiving a blood transfusion immediately after a disaster or languishing, for example. So, in August, Greyshirts began training Ukrainians in point of care ultrasound and whole blood transfusions, among other pre-hospital training topics.
Building Capacity Through Training on Technology: Point of Care Ultrasound
Medical imaging is crucial for treatment in numerous scenarios, but traditionally access to high-quality imaging hasn’t been much of a reality in the field during crisis response. Recent changes in medical technologies, however, have meant the ability to put critical care tools in the hands of field medics.
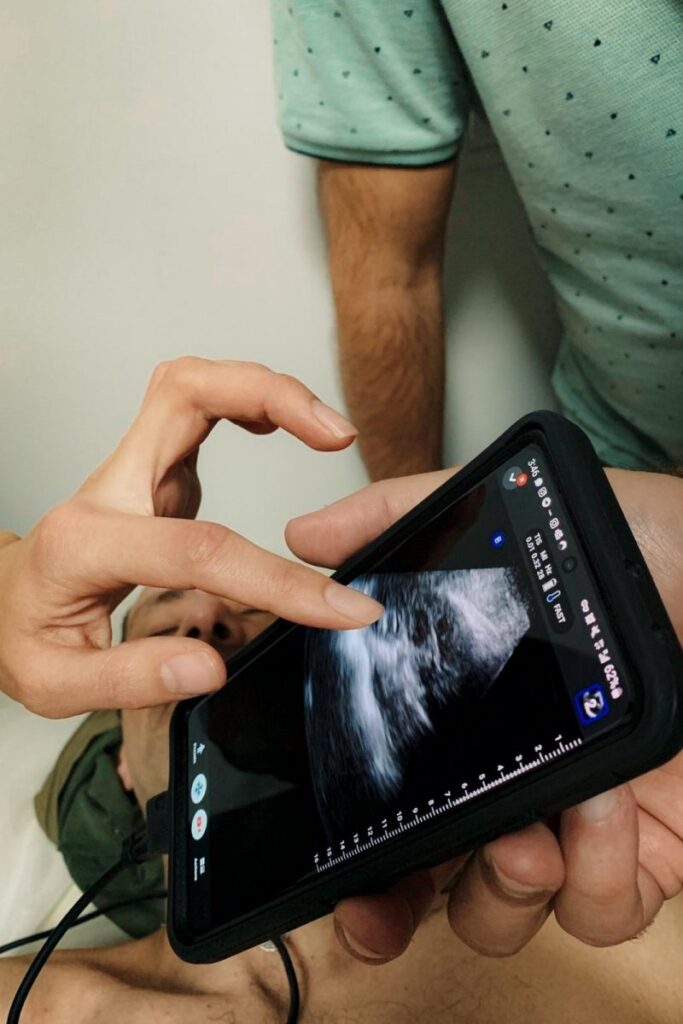
Enter the point of care ultrasound, or POCUS. A POCUS is a handheld probe that connects to a smartphone or tablet. POCUS devices provide real-time imaging via an App, and allow for diagnosing injuries in the field, and help guide procedures that can save lives. Such imaging can help field medical experts treat a variety of issues, including broken bones, collapsed lungs, internal bleeding, cardiac malfunctions, and even OBGYN-related complications. Not only has POCUS revolutionized emergency medical care, it also has the ability to radically transform trauma medicine beyond the hospital walls.
In Ukraine, access to such technology and training on how to use it effectively will empower citizens to provide medical care on the ground in crisis scenarios.
Because POCUS technology is still new, it requires extensive training to use. Team Rubicon Greyshirts in Ukraine trained physicians and paramedics to use the Butterfly iQ+ probe, a handheld POCUS probe that stores images in the Cloud.
In a trauma context, once trained in and equipped with a Butterfly iQ+ probe, medics in the field will be able, for example, to find quick vein access for IVs, provide lung decompression, deliver critical pain relief with nerve block medications, and much more.
Not only were Greyshirts able, over the course of nearly two months, to provide training in POCUS, Team Rubicon also donated 50 Butterfly iQ+ probes—along with a free lifetime subscription to the supporting app—in Ukraine, providing local medical teams with critical access to the life-saving technology long after the international team is gone.
Training in the New and Novel: Whole Blood Transfusions Improve Outcomes
In the U.S. alone, someone needs a blood transfusion every two seconds—approximately 29,000 units of red blood cells are needed every day domestically.
That’s not even in a disaster zone. While typical trauma patients in the U.S. can access a transfusion in time, those in crisis or disaster zones experiencing trauma injuries face far more dire circumstances.

In a hospital context, blood product units require adequate cold storage capacity and timed administration. In the field, neither cold storage nor timed administration is typically available. The solution for decades has been blood transfusion, which was discovered just before WWI. Then, during WWII, U.S. Forces established field blood banks for transfusions on-site, or to go with the patient to the hospital.
In 2010, the Norwegian Navy developed Blood Far Forward, a transfusion concept and method that allows for safe, pre-hospital whole blood transfusions that increase battlefield survival. When field staff are well-trained in buddy transfusion procedures, the risks of disease are low. This is particularly useful in Ukraine, where field medics may encounter battlefield injuries.
In 2020, Ukraine enacted a new law ensuring the safety of blood and blood components donation. To support the new methods and law, Team Rubicon, began training field medics in the critical trauma care tactic this fall.
Knowledge in Action
In less than two months, Greyshirts in Ukraine trained 1,549 individuals in such topics as POCUS and whole blood transfusion, as well as in stop-the-bleed, pre-hospital triage, blast injuries, and treatment of chemical exposure.
Today, bringing such ongoing training and capacity building to Ukraine is having the potential to make a massive impact in the field during this crisis, and far into the future. Training Ukrainians on POCUS and whole blood transfusion will do more than just keep fellow citizens alive in the field, it will help reduce human suffering and the loss of life far into the future.
Want to support Team Rubicon’s international humanitarian aid missions? Here’s how:
-
Donate to disaster response and humanitarian aid operations, domestic or abroad
-
Volunteer domestically to build your skillset for future international work.



